Get your patient on Terazosin Hydrochloride - Terazosin Hydrochloride capsule (Terazosin Hydrochloride)
Terazosin Hydrochloride - Terazosin Hydrochloride capsule prescribing information
INDICATIONS AND USAGE
Terazosin capsules, USP are indicated for the treatment of symptomatic benign prostatic hyperplasia (BPH). There is a rapid response, with approximately 70% of patients experiencing an increase in urinary flow and improvement in symptoms of BPH when treated with terazosin capsules, USP. The long-term effects of terazosin capsules, USP on the incidence of surgery, acute urinary obstruction or other complications of BPH are yet to be determined.
Terazosin capsules, USP are also indicated for the treatment of hypertension. Terazosin capsules, USP can be used alone or in combination with other antihypertensive agents such as diuretics or beta-adrenergic blocking agents.
DOSAGE AND ADMINISTRATION
If terazosin capsules administration is discontinued for several days, therapy should be reinstituted using the initial dosing regimen.
Benign Prostatic Hyperplasia
Initial Dose
1 mg at bedtime is the starting dose for all patients, and this dose should not be exceeded as an initial dose. Patients should be closely followed during initial administration in order to minimize the risk of severe hypotensive response.
Subsequent Doses
The dose should be increased in a stepwise fashion to 2 mg, 5 mg, or 10 mg once daily to achieve the desired improvement of symptoms and/or flow rates. Doses of 10 mg once daily are generally required for the clinical response. Therefore, treatment with 10 mg for a minimum of 4 to 6 weeks may be required to assess whether a beneficial response has been achieved. Some patients may not achieve a clinical response despite appropriate titration. Although some additional patients responded at a 20 mg daily dose, there was an insufficient number of patients studied to draw definitive conclusions about this dose. There are insufficient data to support the use of higher doses for those patients who show inadequate or no response to 20 mg daily. If terazosin administration is discontinued for several days or longer, therapy should be reinstituted using the initial dosing regimen.
Use With Other Drugs
Caution should be observed when terazosin capsules are administered concomitantly with other antihypertensive agents, especially the calcium channel blocker verapamil, to avoid the possibility of developing significant hypotension. When using terazosin capsules and other antihypertensive agents concomitantly, dosage reduction and retitration of either agent may be necessary (see PRECAUTIONS ). Hypotension has been reported when terazosin capsules have been used with phosphodiesterase-5 (PDE-5) inhibitors.
Hypertension
The dose of terazosin capsules and the dose interval (12 or 24 hours) should be adjusted according to the patient’s individual blood pressure response. The following is a guide to its administration:
Initial Dose
1 mg at bedtime is the starting dose for all patients, and this dose should not be exceeded. This initial dosing regimen should be strictly observed to minimize the potential for severe hypotensive effects.
Subsequent Doses
The dose may be slowly increased to achieve the desired blood pressure response. The usual recommended dose range is 1 mg to 5 mg administered once a day; however, some patients may benefit from doses as high as 20 mg per day. Doses over 20 mg do not appear to provide further blood pressure effect and doses over 40 mg have not been studied. Blood pressure should be monitored at the end of the dosing interval to be sure control is maintained throughout the interval. It may also be helpful to measure blood pressure 2 to 3 hours after dosing to see if the maximum and minimum responses are similar, and to evaluate symptoms such as dizziness or palpitations which can result from excessive hypotensive response. If response is substantially diminished at 24 hours an increased dose or use of a twice daily regimen can be considered. If terazosin administration is discontinued for several days or longer, therapy should be reinstituted using the initial dosing regimen. In clinical trials, except for the initial dose, the dose was given in the morning.
Use With Other Drugs
(See above.)
CONTRAINDICATIONS
Terazosin capsules are contraindicated in patients known to be hypersensitive to terazosin hydrochloride.
ADVERSE REACTIONS
Benign Prostatic Hyperplasia
The incidence of treatment-emergent adverse events has been ascertained from clinical trials conducted worldwide. All adverse events reported during these trials were recorded as adverse reactions. The incidence rates presented below are based on combined data from six placebo-controlled trials involving once-a-day administration of terazosin capsules at doses ranging from 1 to 20 mg. Table 1 summarizes those adverse events reported for patients in these trials when the incidence rate in the terazosin group was at least 1%, and was greater than that for the placebo group, or where the reaction is of clinical interest. Asthenia, postural hypotension, dizziness, somnolence, nasal congestion/rhinitis, and impotence were the only events that were significantly (p ≤ 0.05) more common in patients receiving terazosin capsules than in patients receiving placebo. The incidence of urinary tract infection was significantly lower in the patients receiving terazosin capsules than in patients receiving placebo. An analysis of the incidence rate of hypotensive adverse events (see PRECAUTIONS ) adjusted for the length of drug treatment has shown that the risk of the events is greatest during the initial seven days of treatment, but continues at all time intervals.
Body System | Terazosin (N = 636) | Placebo (N = 360) |
BODY AS A WHOLE | ||
Asthenia Flu Syndrome Headache | 7.4% • 2.4% 4.9% | 3.3% 1.7% 5.8% |
CARDIOVASCULAR SYSTEM | ||
Hypotension Palpitations Postural Hypotension Syncope | 0.6% 0.9% 3.9% • 0.6% | 0.6% 1.1% 0.8% 0.0% |
DIGESTIVE SYSTEM | ||
Nausea | 1.7% | 1.1% |
METABOLIC AND NUTRITIONAL DISORDERS | ||
Peripheral Edema Weight Gain | 0.9% 0.5% | 0.3% 0.0% |
NERVOUS SYSTEM | ||
Dizziness Somnolence Vertigo | 9.1% • 3.6% • 1.4% | 4.2% 1.9% 0.3% |
RESPIRATORY SYSTEM | ||
Dyspnea Nasal Congestion/Rhinitis | 1.7% 1.9% • | 0.8% 0.0% |
SPECIAL SENSES | ||
Blurred Vision/Amblyopia | 1.3% | 0.6% |
UROGENITAL SYSTEM | ||
Impotence Urinary Tract Infection | 1.6% • 1.3% | 0.6% 3.9% • |
†Includes weakness, tiredness, lassitude, and fatigue.
•p ≤ 0.05 comparison between groups.
Additional adverse events have been reported, but these are, in general, not distinguishable from symptoms that might have occurred in the absence of exposure to terazosin. The safety profile of patients treated in the long-term open-label study was similar to that observed in the controlled studies.
The adverse events were usually transient and mild or moderate in intensity, but sometimes were serious enough to interrupt treatment. In the placebo-controlled clinical trials, the rates of premature termination due to adverse events were not statistically different between the placebo and terazosin groups. The adverse events that were bothersome, as judged by their being reported as reasons for discontinuation of therapy by at least 0.5% of the terazosin group and being reported more often than in the placebo group, are shown in Table 2.
Body System | Terazosin (N = 636) | Placebo (N = 360) |
BODY AS A WHOLE | ||
Fever Headache | 0.5% 1.1% | 0.0% 0.8% |
CARDIOVASCULAR SYSTEM | ||
Postural Hypotension Syncope | 0.5% 0.5% | 0.0% 0.0% |
DIGESTIVE SYSTEM | ||
Nausea | 0.5% | 0.3% |
NERVOUS SYSTEM | ||
Dizziness Vertigo | 2.0% 0.5% | 1.1% 0.0% |
RESPIRATORY SYSTEM | ||
Dyspnea | 0.5% | 0.3% |
SPECIAL SENSES | ||
Blurred Vision/Amblyopia | 0.6% | 0.0% |
UROGENITAL SYSTEM | ||
Urinary Tract Infection | 0.5% | 0.3% |
Hypertension
The prevalence of adverse reactions has been ascertained from clinical trials conducted primarily in the United States. All adverse experiences (events) reported during these trials were recorded as adverse reactions. The prevalence rates presented below are based on combined data from fourteen placebo-controlled trials involving once-a-day administration of terazosin capsules, as monotherapy or in combination with other antihypertensive agents, at doses ranging from 1 to 40 mg. Table 3 summarizes those adverse experiences reported for patients in these trials where the prevalence rate in the terazosin group was at least 5%, where the prevalence rate for the terazosin group was at least 2% and was greater than the prevalence rate for the placebo group, or where the reaction is of particular interest. Asthenia, blurred vision, dizziness, nasal congestion, nausea, peripheral edema, palpitations and somnolence were the only symptoms that were significantly (p < 0.05) more common in patients receiving terazosin capsules than in patients receiving placebo. Similar adverse reaction rates were observed in placebo-controlled monotherapy trials.
Body System | Terazosin (N = 859) | Placebo (N = 506) |
BODY AS A WHOLE | ||
†Asthenia Back Pain Headache | 11.3% • 2.4% 16.2% | 4.3% 1.2% 15.8% |
CARDIOVASCULAR SYSTEM | ||
Palpitations Postural Hypotension Tachycardia | 4.3% • 1.3% 1.9% | 1.2% 0.4% 1.2% |
DIGESTIVE SYSTEM | ||
Nausea | 4.4% • | 1.4% |
METABOLIC AND NUTRITIONAL DISORDERS | ||
Edema Peripheral Edema Weight Gain | 0.9% 5.5% • 0.5% | 0.6% 2.4% 0.2% |
MUSCULOSKELETAL SYSTEM | ||
Pain – Extremities | 3.5% | 3.0% |
NERVOUS SYSTEM | ||
Depression Dizziness Libido Decreased Nervousness Paresthesia Somnolence | 0.3% 19.3% • 0.6% 2.3% 2.9% 5.4% • | 0.2% 7.5% 0.2% 1.8% 1.4% 2.6% |
RESPIRATORY SYSTEM | ||
Dyspnea Nasal Congestion Sinusitis | 3.1% 5.9% • 2.6% | 2.4% 3.4% 1.4% |
SPECIAL SENSES | ||
Blurred Vision | 1.6% • | 0.0% |
UROGENITAL SYSTEM | ||
Impotence | 1.2% | 1.4% |
†Includes weakness, tiredness, lassitude, and fatigue.
•Statistically significant at p=0.05 level.
Additional adverse reactions have been reported, but these are, in general, not distinguishable from symptoms that might have occurred in the absence of exposure to terazosin capsules. The following additional adverse reactions were reported by at least 1% of 1987 patients who received terazosin in controlled or open, short- or long-term clinical trials studies or have been reported during marketing experience:
Body as a Whole
Chest pain, facial edema, fever, abdominal pain, neck pain, shoulder pain.
Cardiovascular System
Arrhythmia, vasodilation.
Digestive System
Constipation, diarrhea, dry mouth, dyspepsia, flatulence, vomiting.
Metabolic/Nutritional Disorders
Gout.
Musculoskeletal System
Arthralgia, arthritis, joint disorder, myalgia.
Nervous System
Anxiety, insomnia.
Respiratory System
Bronchitis, cold symptoms, epistaxis, flu symptoms, increased cough, pharyngitis, rhinitis.
Skin and Appendages
Pruritus, rash, sweating.
Special Senses
Abnormal vision, conjunctivitis, tinnitus.
Urogenital System
Urinary frequency, urinary incontinence primarily reported in postmenopausal women, urinary tract infection.
The adverse reactions were usually mild or moderate in intensity but sometimes were serious enough to interrupt treatment. The adverse reactions that were most bothersome, as judged by their being reported as reasons for discontinuation of therapy by at least 0.5% of the terazosin group and being reported more often than in the placebo group, are shown in Table 4.
Body System | Terazosin (N = 859) | Placebo (N = 506) |
BODY AS A WHOLE | ||
Asthenia Headache | 1.6% 1.3% | 0.0% 1.0% |
CARDIOVASCULAR SYSTEM | ||
Palpitations Postural Hypotension Syncope Tachycardia | 1.4% 0.5% 0.5% 0.6% | 0.2% 0.0% 0.2% 0.0% |
DIGESTIVE SYSTEM | ||
Nausea | 0.8% | 0.0% |
METABOLIC AND NUTRITIONAL DISORDERS | ||
Peripheral Edema | 0.6% | 0.0% |
NERVOUS SYSTEM | ||
Dizziness Paresthesia Somnolence | 3.1% 0.8% 0.6% | 0.4% 0.2% 0.2% |
RESPIRATORY SYSTEM | ||
Dyspnea Nasal Congestion | 0.9% 0.6% | 0.6% 0.0% |
SPECIAL SENSES | ||
Blurred Vision | 0.6% | 0.0% |
Post-marketing Experience
Post-marketing experience indicates that in rare instances patients may develop allergic reactions, including anaphylaxis, following administration of terazosin hydrochloride. There have been reports of priapism and thrombocytopenia during post-marketing surveillance. Atrial fibrillation has been reported.
During cataract surgery, a variant of small pupil syndrome known as Intraoperative Floppy Iris Syndrome (IFIS) has been reported in association with alpha-1 blocker therapy (see PRECAUTIONS ).
Drug Interactions
In controlled trials, terazosin capsules have been added to diuretics, and several beta-adrenergic blockers; no unexpected interactions were observed. Terazosin capsules have also been used in patients on a variety of concomitant therapies; while these were not formal interaction studies, no interactions were observed. Terazosin capsules have been used concomitantly in at least 50 patients on the following drugs or drug classes:
- analgesic/anti-inflammatory (e.g., acetaminophen, aspirin, codeine, ibuprofen, indomethacin);
- antibiotics (e.g., erythromycin, trimethoprim and sulfamethoxazole);
- anticholinergic/sympathomimetics (e.g., phenylephrine hydrochloride, phenylpropanolamine hydrochloride, pseudoephedrine hydrochloride);
- antigout (e.g., allopurinol);
- antihistamines (e.g., chlorpheniramine);
- cardiovascular agents (e.g., atenolol, hydrochlorothiazide, methyclothiazide, propranolol);
- corticosteroids;
- gastrointestinal agents (e.g., antacids);
- hypoglycemics
- sedatives and tranquilizers (e.g., diazepam).
DESCRIPTION
Terazosin hydrochloride, an alpha-1-selective adrenoceptor blocking agent, is a quinazoline derivative represented by the following chemical name, molecular formula and structural formula: (RS)-Piperazine, 1-(4-amino-6,7-dimethoxy-2-quinazolinyl)-4-[(tetrahydro-2-furanyl)carbonyl]-, monohydrochloride, C 19 H 26 ClN 5 O 4 . It has the following structural formula:
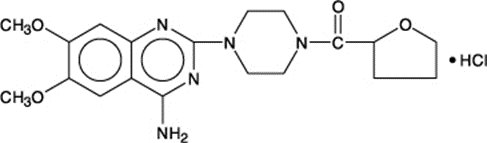
Terazosin hydrochloride is a white, crystalline substance, freely soluble in water and isotonic saline and has a molecular weight of 423.93. Terazosin capsules, USP, for oral administration, are supplied in four dosage strengths containing terazosin hydrochloride, USP equivalent to 1 mg, 2 mg, 5 mg, or 10 mg of terazosin. Inactive ingredients: Crospovidone, lactose (monohydrate), magnesium stearate, and microcrystalline cellulose. The capsule shells and imprinting inks contain: D & C Yellow #10 Aluminum Lake, FD & C Blue #1 Aluminum Lake, FD & C Blue #2 Aluminum Lake, FD & C Red #40 Aluminum Lake, gelatin, propylene glycol, shellac, synthetic black iron oxide, and titanium dioxide. The 5 mg also contains: D & C Red #28.
CLINICAL PHARMACOLOGY
Pharmacodynamics
A. Benign Prostatic Hyperplasia (BPH)
The symptoms associated with BPH are related to bladder outlet obstruction, which is comprised of two underlying components: a static component and a dynamic component. The static component is a consequence of an increase in prostate size. Over time, the prostate will continue to enlarge. However, clinical studies have demonstrated that the size of the prostate does not correlate with the severity of BPH symptoms or the degree of urinary obstruction. The dynamic component is a function of an increase in smooth muscle tone in the prostate and bladder neck, leading to constriction of the bladder outlet. Smooth muscle tone is mediated by sympathetic nervous stimulation of alpha-1 adrenoceptors, which are abundant in the prostate, prostatic capsule and bladder neck. The reduction in symptoms and improvement in urine flow rates following administration of terazosin is related to relaxation of smooth muscle produced by blockade of alpha-1 adrenoceptors in the bladder neck and prostate. Because there are relatively few alpha-1 adrenoceptors in the bladder body, terazosin is able to reduce the bladder outlet obstruction without affecting bladder contractility.
Terazosin has been studied in 1222 men with symptomatic BPH. In three placebo-controlled studies, symptom evaluation and uroflowmetric measurements were performed approximately 24 hours following dosing. Symptoms were quantified using the Boyarsky Index. The questionnaire evaluated both obstructive (hesitancy, intermittency, terminal dribbling, impairment of size and force of stream, sensation of incomplete bladder emptying) and irritative (nocturia, daytime frequency, urgency, dysuria) symptoms by rating each of the 9 symptoms from 0 to 3, for a total score of 27 points. Results from these studies indicated that terazosin statistically significantly improved symptoms and peak urine flow rates over placebo as follows:
| Symptom score (Range 0-27) | Peak Flow rate (ml/sec) | |||||
| N | Mean Baseline | Mean change (%) | N | Mean Baseline | Mean change (%) | |
Study 1 (10mg) a Titration to fixed dose (12 wks) | ||||||
Placebo Terazosin | 55 54 | 9.7 10.1 | -2.3 (24) -4.5 (45) • | 54 52 | 10.1 8.8 | +1.0 (10) +3.0 (34) • |
| Study 2 (2,5,10,20 mg) b Titration to response (24wks) | ||||||
Placebo Terazosin | 89 85 | 12.5 12.2 | -3.8 (30) -5.3 (43) • | 88 84 | 8.8 8.4 | +1.4 (16) +2.9 (35) • |
Study 3 (1, 2, 5, 10 mg) c Titration to response (24 wks) | ||||||
Placebo Terazosin | 74 73 | 10.4 10.9 | -1.1 (11) -4.6 (42) • | 74 73 | 8.8 8.6 | +1.2 (14) +2.6 (30) |
• Significantly (p ≤ 0.05) more improvement than placebo.
a Highest dose 10 mg shown.
b 23% of patients on 10 mg, 41% of patients on 20 mg.
c 67% of patients on 10 mg
In all three studies, both symptom scores and peak urine flow rates showed statistically significant improvement from baseline in patients treated with terazosin capsules from week 2 (or the first clinic visit) and throughout the study duration.
Analysis of the effect of terazosin capsules on individual urinary symptoms demonstrated that compared to placebo, terazosin capsules significantly improved the symptoms of hesitancy, intermittency, impairment in size and force of urinary stream, sensation of incomplete emptying, terminal dribbling, daytime frequency and nocturia.
Global assessments of overall urinary function and symptoms were also performed by investigators who were blinded to patient treatment assignment. In studies 1 and 3, patients treated with terazosin capsules had a significantly (p ≤ 0.001) greater overall improvement compared to placebo treated patients.
In a short term study (Study 1), patients were randomized to either 2, 5 or 10 mg of terazosin capsules or placebo. Patients randomized to the 10 mg group achieved a statistically significant response in both symptoms and peak flow rate compared to placebo (Figure 1).
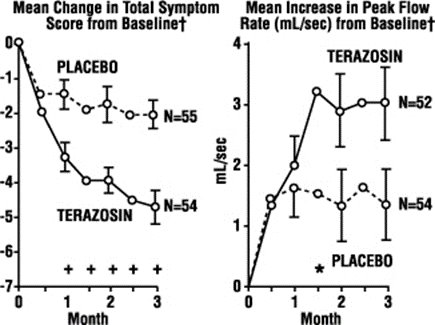
FIGURE1, STUDY1
† for baseline values see above table
• p ≤ 0.05, compared to placebo group
In a long-term, open-label, non-placebo controlled clinical trial, 181 men were followed for 2 years and 58 of these men were followed for 30 months. The effect of terazosin capsules on urinary symptom scores and peak flow rates was maintained throughout the study duration (Figures 2 and 3):
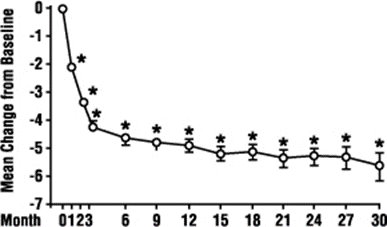
FIGURE 2. Mean Change in Total Symptom Score from Baseline Long-Term, Open-Label, Non-Placebo Controlled Study (N=494)
• p ≤ 0.05 vs. baseline; mean baseline = 10.7
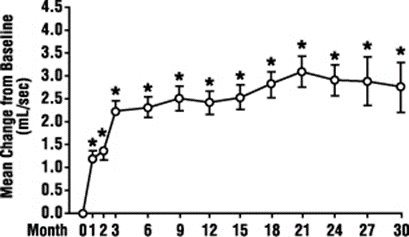
FIGURE 3. Mean Change in Peak Flow Rate from Baseline Long-Term, Open-Label, Non-Placebo Controlled Study (N=494)
•p ≤ 0.05 vs. baseline; mean baseline = 9.9
In this long-term trial, both symptom scores and peak urinary flow rates showed statistically significant improvement suggesting a relaxation of smooth muscle cells.
Although blockade of alpha-1 adrenoceptors also lowers blood pressure in hypertensive patients with increased peripheral vascular resistance, terazosin treatment of normotensive men with BPH did not result in a clinically significant blood pressure lowering effect:
| Group | Normotensive Patients DBP ≤ 90 mm Hg | Hypertensive Patients DBP > 90 mm Hg | |||
| N | Mean change | N | Mean change | ||
SBP (mm Hg) | Placebo Terazosin | 293 519 | -0.1 -3.3 • | 45 65 | -5.8 -14.4 • |
DBP (mm Hg) | Placebo Terazosin | 293 519 | +0.4 -2.2 • | 45 65 | -7.1 -15.1 • |
•p ≤ 0.05 vs. placebo
B. Hypertension
In animals, terazosin causes a decrease in blood pressure by decreasing total peripheral vascular resistance. The vasodilatory hypotensive action of terazosin appears to be produced mainly by blockade of alpha-1 adrenoceptors. Terazosin decreases blood pressure gradually within 15 minutes following oral administration.
Patients in clinical trials of terazosin were administered once daily (the great majority) and twice daily regimens with total doses usually in the range of 5 to 20 mg/day, and had mild (about 77%, diastolic pressure 95 to 105 mmHg) or moderate (23%, diastolic pressure 105 to 115 mmHg) hypertension. Because terazosin, like all alpha antagonists, can cause unusually large falls in blood pressure after the first dose or first few doses, the initial dose was 1 mg in virtually all trials, with subsequent titration to a specified fixed dose or titration to some specified blood pressure end point (usually a supine diastolic pressure of 90 mmHg).
Blood pressure responses were measured at the end of the dosing interval (usually 24 hours) and effects were shown to persist throughout the interval, with the usual supine responses 5 to 10 mmHg systolic and 3.5 to 8 mmHg diastolic greater than placebo. The responses in the standing position tended to be somewhat larger, by 1 to 3 mmHg, although this was not true in all studies. The magnitude of the blood pressure responses was similar to prazosin and less than hydrochlorothiazide (in a single study of hypertensive patients). In measurements 24 hours after dosing, heart rate was unchanged.
Limited measurements of peak response (2 to 3 hours after dosing) during chronic terazosin administration indicate that it is greater than about twice the trough (24 hour) response, suggesting some attenuation of response at 24 hours, presumably due to a fall in blood terazosin concentrations at the end of the dose interval. This explanation is not established with certainty, however, and is not consistent with the similarity of blood pressure response to once daily and twice daily dosing and with the absence of an observed dose-response relationship over a range of 5 to 20 mg, i.e., if blood concentrations had fallen to the point of providing less than full effect at 24 hours, a shorter dosing interval or larger dose should have led to increased response.
Further dose response and dose duration studies are being carried out. Blood pressure should be measured at the end of the dose interval; if response is not satisfactory, patients may be tried on a larger dose or twice daily dosing regimen. The latter should also be considered if possibly blood pressure-related side effects, such as dizziness, palpitations, or orthostatic complaints, are seen within a few hours after dosing.
The greater blood pressure effect associated with peak plasma concentrations (first few hours after dosing) appears somewhat more position-dependent (greater in the erect position) than the effect of terazosin at 24 hours and in the erect position there is also a 6 to 10 beat per minute increase in heart rate in the first few hours after dosing. During the first 3 hours after dosing 12.5% of patients had a systolic pressure fall of 30 mmHg or more from supine to standing, or standing systolic pressure below 90 mmHg with a fall of at least 20 mmHg, compared to 4% of a placebo group.
There was a tendency for patients to gain weight during terazosin therapy. In placebo-controlled monotherapy trials, male and female patients receiving terazosin gained a mean of 1.7 and 2.2 pounds respectively, compared to losses of 0.2 and 1.2 pounds respectively in the placebo group. Both differences were statistically significant.
During controlled clinical trials, patients receiving terazosin monotherapy had a small but statistically significant decrease (a 3% fall) compared to placebo in total cholesterol and the combined low-density and very-low-density lipoprotein fractions. No significant changes were observed in high-density lipoprotein fraction and triglycerides compared to placebo.
Analysis of clinical laboratory data following administration of terazosin suggested the possibility of hemodilution based on decreases in hematocrit, hemoglobin, white blood cells, total protein and albumin. Decreases in hematocrit and total protein have been observed with alpha-blockade and are attributed to hemodilution.
Pharmacokinetics
Terazosin Hydrochloride administered as capsules is essentially completely absorbed in man. Administration of capsules immediately after meals had a minimal effect on the extent of absorption. The time to reach peak plasma concentration however, was delayed by about 40 minutes. Terazosin has been shown to undergo minimal hepatic first-pass metabolism and nearly all of the circulating dose is in the form of parent drug. The plasma levels peak about one hour after dosing, and then decline with a half-life of approximately 12 hours. In a study that evaluated the effect of age on terazosin pharmacokinetics, the mean plasma half-lives were 14.0 and 11.4 hours for the age group ≥ 70 years and the age group of 20 to 39 years, respectively. After oral administration the plasma clearance was decreased by 31.7% in patients 70 years of age or older compared to that in patients 20 to 39 years of age.
The drug is 90 to 94% bound to plasma proteins and binding is constant over the clinically observed concentration range. Approximately 10% of an orally administered dose is excreted as parent drug in the urine and approximately 20% is excreted in the feces. The remainder is eliminated as metabolites. Impaired renal function had no significant effect on the elimination of terazosin, and dosage adjustment of terazosin to compensate for the drug removal during hemodialysis (approximately 10%) does not appear to be necessary. Overall, approximately 40% of the administered dose is excreted in the urine and approximately 60% in the feces. The disposition of the compound in animals is qualitatively similar to that in man.
HOW SUPPLIED
Terazosin Capsules, USP are available as:
1 mg : White capsules imprinted AP 781 in black ink, filled with white powder are supplied as follows:
NDC 24689-792-03 bottles of 90 capsules
NDC 24689-792-01 bottles of 100 capsules
NDC 24689-792-10 bottles of 1000 capsules
2 mg : Yellow capsules imprinted AP 782 in black ink, filled with white powder are supplied as follows:
NDC 24689-855-03 bottles of 90 capsules
NDC 24689-855-01 bottles of 100 capsules
NDC 24689-855-10 bottles of 1000 capsules
5 mg : Pink capsules imprinted AP 783 in black ink, filled with white powder are supplied as follows:
NDC 24689-882-03 bottles of 90 capsules
NDC 24689-882-01 bottles of 100 capsules
NDC 24689-882-10 bottles of 1000 capsules
10 mg : Aqua capsules imprinted AP 784 in black ink, filled with white powder are supplied as follows:
NDC 24689-961-03 bottles of 90 capsules
NDC 24689-961-01 bottles of 100 capsules
NDC 24689-961-10 bottles of 1000 capsules
Store at 20° to 25°C (68° to 77°F) [see USP Controlled Room Temperature]. Protect from light and moisture.
Dispense in a tight, light-resistant container.
Rx only
Manufactured for:
Apnar Pharma LP
Chino, CA, USA 91710
Rev. 01/2025